By: Bruce W. McCollum, MHA
My job is to blend the clinical with the business end of care. In so doing, I examine initiatives being used to treat ill and injured parties and make recommendations for how care can be enhanced. This article is about day time initiatives aimed at those with brain injuries.
Across America and Canada, we are seeing more and more of these programs, sometimes blended into large assisted living and memory care communities. Those served include those who are victims of falls and other home accidents, crime, auto and work accidents and strokes. The results are measurable, and patients are benefiting.
However, there is one caveat: We must be careful to segregate patient populations based upon their level of function. If the modalities used for a low functioning patient are the same for a high functioning one, our effectiveness can be legitimately questioned. We also run the risk of alienating those who feel their specific levels of function are being ignored.
Now, on to the meat of my article…
Daytime neurological cognitive programs are often designed to support individuals who have sustained injuries but continue to demonstrate high intellectual functioning. Neurologists and other specialty physicians refer to these programs all the time as a part of a patient’s long-term neurological improvement.
These specialized programs aim to enhance cognitive abilities, improve quality of life, and facilitate a more effective recovery process. Here’s a comprehensive analysis of how these programs can be significantly beneficial, along with specific examples to illustrate their effectiveness.
1. Enhanced Cognitive Rehabilitation
Example: A 35-year-old software engineer suffered a traumatic brain injury (TBI) in a car accident. Despite his injury, he retained his intellectual capabilities but struggled with attention and memory. A daytime cognitive program tailored to his needs included memory exercises, problem-solving tasks, and attention-enhancing activities. Over time, he reported improved memory recall and a better ability to focus on complex tasks at work.
2. Social Interaction and Emotional Support
Example: A young woman with a spinal cord injury participated in a group-based cognitive program. Despite her physical limitations, her intellectual functioning remained intact.
The program provided not only cognitive exercises but also a platform for social interaction. Engaging with peers facing similar challenges helped her combat feelings of isolation and depression, significantly improving her emotional well-being. In documenting her participation for guardians, insurers, physicians and others, skilled staff should note her response to certain activity and how it compares to a previous reporting period. The focus must be on outcomes.

3. Structured Routine and Sense of Purpose
Example: A veteran with mild cognitive impairment due to a service-related injury found it challenging to maintain a structured daily routine. The daytime program offered a consistent schedule filled with cognitive tasks, physical activities, and skill-building sessions. This structure provided him with a sense of purpose and a routine that mimicked a workday, contributing to an improved sense of self-worth and independence.
4. Personalized Cognitive Development
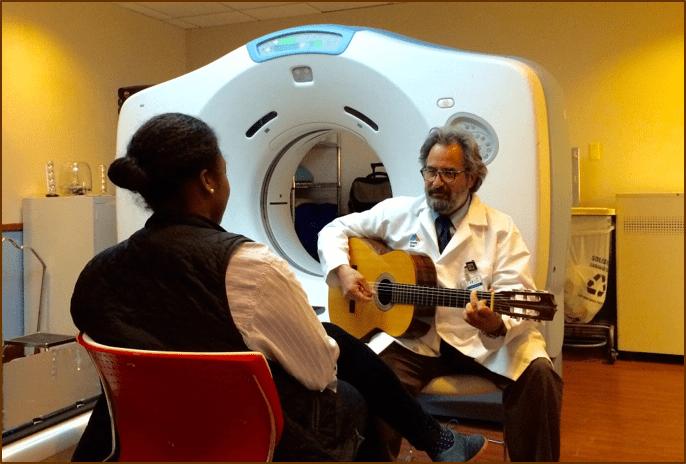
Example: A professional pianist suffered a mild stroke, affecting her hand coordination and cognitive speed. A personalized program was developed, focusing on music therapy and cognitive exercises related to her profession. This targeted approach not only aided in her physical rehabilitation but also kept her intellectually stimulated and engaged with her passion, fostering a more positive and motivated mindset toward recovery.
In documenting this for insurers, guardians, physicians and others, the provider should note specific responses and explain tools for measuring improvement on a consistent basis.
5. Incorporation of Technology and Innovation
Example: A young adult with a concussion from a sports injury used a cognitive program that incorporated virtual reality (VR) technology. The VR scenarios were designed to improve his spatial awareness, reaction time, and decision-making skills. This innovative approach made the rehabilitation process more engaging and closely mirrored real-life situations he would encounter, enhancing the practical benefits of his recovery.

6. Family Involvement and Education
Example: A mother of two suffered a brain injury but remained highly functional intellectually. The program she attended offered family education sessions, teaching her family how to support her recovery at home. This not only empowered her support system but also ensured that her home environment was conducive to her cognitive and emotional well-being. Caregiver preparedness must be a part of a neurologically focused cognitive treatment program.

In Summary my friends…
Daytime neurological cognitive programs offer a beacon of hope and progress for individuals who have sustained injuries yet remain intellectually vibrant. Through personalized and innovative approaches, these programs provide the tools and support necessary for individuals to navigate their recovery journey effectively.
They foster an environment where healing is not just about physical recovery but also about regaining cognitive strength, emotional resilience, and a sense of purpose in life. As more research unfolds and technology advances, these programs will undoubtedly continue to evolve, offering even more targeted and effective support for those in need without hospitalizations.
Let’s just make sure our programs reach the level of quality required to accomplish these lofty goals.
Another Blog Post by Direct Care Training & Resource Center, Inc. Photos used are designed to complement the written content. They do not imply a relationship with or endorsement by any individual nor entity and may belong to their respective copyright holders.
| Follow us in the Social Stratosphere… | ||||
|
|